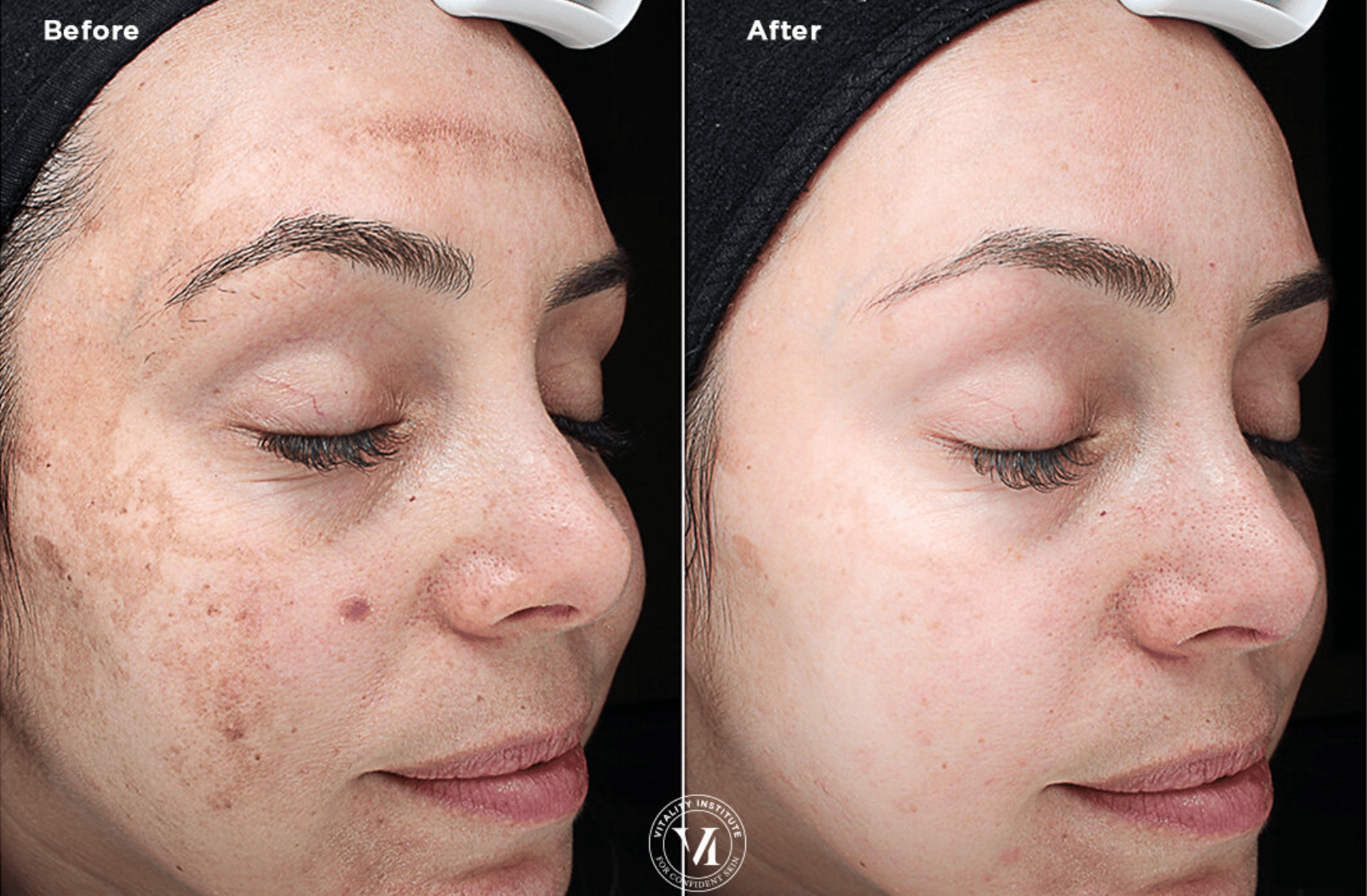
What is Hyper Pigmentation?
Hyperpigmentation is the term that refers to a variety of dark spots that can appear on our skin. These can be further broken down into categories and have a variety of contributors. All skin can be affected and are susceptible to hyperpigmentation, however, medium to darker skin tones are more prone to developing these color variations.
Changes in the color of the skin can result from various causes or combinations both internal and external. Internal causes include hormones and inflammatory diseases of the skin such as eczema, psoriasis, and medications (Wang et al., 2021). The most evident external cause is UV exposure. Sun exposure stimulates melanocyte cells, which produce the pigment also known as melanin, in our skin and eyes. We all have the same number of melanocytes, however, people with medium to darker skin produce more melanin than those with lighter skin. The pigment is produced in the innermost layer of the skin and near the iris of the eye. Given this information sun block and ultraviolet (UV), eye protection is essential in the prevention of sun damage!
Why is Sunblock So Important?
Sun block should be utilized not only to prevent skin cancer but to prevent uneven skin tone that results from sun damage. Fair-skinned individuals typically develop a routine that includes daily application of SPF to avoid skin cancer as they are aware of their susceptibility. Darker-skinned individuals often fail to realize that they are also susceptible to skin cancer. Melanin protects the skin by redistributing the absorbed UV rays into the upper layers of the skin, preventing oxidative stress and damage to DNA but it is not a substitute for sunscreen (Goon et al., 2021). It is this misconception that contributes not only to the development of skin cancer but also to hyperpigmentation.
What are the Types of Hyperpigmentation?
There are a variety of different types of hyperpigmentation known as freckles, age spots, post-inflammatory hyperpigmentation, and Melasma. Freckles develop in lighter-skinned individuals as a response to the overproduction of melanin pigmentation related to sun exposure. There are two types of freckles, ephelides and solar lentigines (sun spots). Ephelides are what we traditionally think of when we visualize freckles. They can come on in youth, are 1-2mm in size with irregular borders, and tend to fade as we age (Praetorius et al., 2014). Sun spots, also known as lentigines, age spots, or liver spots develop after the age of forty in individuals with medium to dark skin. They are larger in size, have regular borders, and are a result of exposure to the sun over time (Praetorius et al., 2014).
There is no treatment that will completely eliminate freckles but it is possible to minimize their appearance with the use of sunblock and hats. Starting these preventive practices early will certainly reduce the number of sunspots as we age.
Post-inflammatory Hyperpigmentation
Post-inflammatory hyperpigmentation (PIH) describes what happens to skin that has been injured. Essentially, the injury causes an inflammatory response that stimulates the production of melanin causing the production of pigment and in turn darkening of the skin. Inflammatory skin conditions such as acne, lupus, eczema, or psoriasis can trigger overproduction of melanin causing areas of the skin to further darken. The same skin types that are prone to excess pigmentation are most likely to experience post-inflammatory hyperpigmentation thus sun exposure can worsen the effect. It is possible to decrease the risk of PIH by not excessively picking, squeezing, or scratching the skin. If dark areas persist there are several options to lighten the skin most of which require medical background and knowledge of suitable products. Do not go it alone, consult a professional.
Melasma
Melasma is the most complex type of hyperpigmentation. Its course of treatment can be unpredictable and relapse is very common making it a very distressing condition for those who have it. All aspects of its cause are not fully established, but continue to be researched. To date, no single therapeutic approach has been proven entirely effective (Wang et al., 2021).
The darker skin of melasma is large and extremely irregular. The known causes include a complex interaction between genetics, sex hormones, and sun exposure. It is important to keep in mind that heat, certain medications, and inflammatory skin conditions also exacerbate melasma and to avoid these whenever possible. UV exposure causes increased melanin production which can be accelerated through hormones and/or medications. Chronic UV exposure leads to photo-aging, oxidative stress, and inflammation that contribute to the sustained melanogenesis observed in melasma (Esposito et al., 2022). Melasma is most prevalent among Hispanics, African Americans, Asians, or Middle Eastern females, and tends to present in patients between the ages of 20 to 40 (Gonzalez et al., 2022).
Preventing Melasma
Prevention of melasma is first and foremost accomplished through utilizing the correct type and regular application of sunscreen. Physical sunblock with zinc oxide and or titanium dioxide rather than a chemical sunscreen is the most important factor when choosing an effective SPF. Physical ingredients deflect ultraviolet radiation. Chemical sunscreens absorb UV rays into the skin and convert the rays into heat which are then released by the skin. Allowing the rays into the skin and having heat production causes inflammation which increases the skin’s production of pigmentation and in turn permanently darkening of the skin. Removing all of the triggers that increase melanin production is the first step to preventing this condition, beginning with proper sunblock.
A 2019 study of 100 participants with melasma applied physical sunblock every 3 hours during the day for 12 weeks. All 100 participants saw a reduction in the dark spots currently present (Wang et al., 2021). This study clearly demonstrated frequent application of physical SPF alone is an effective preventive treatment.
Depigmenting Agents
Depigmenting agents aka skin lighteners are another recommended modality. Antioxidants and skin lighteners aim to block the tyrosinase enzyme pathway to prevent the production of additional pigmentation. Providing antioxidants to the skin and moisturizers help improve the protective skin barrier and also prevent further damage. In addition to at-home treatments to remove the top layers of the epidermis in-office procedures such as chemical peels and micro-needling can be implemented and performed by a licensed professional to further assist in treatment.
As previously stated, this is a complex condition that requires a dedicated regimen. Since the pigmentation can be in all layers of the skin, the time it takes to see a change in addition to the level of commitment required can be frustrating. Melasma does not have a cure, but rather requires ongoing management or it will likely resurface.
Take Care of Your Skin
The skin is our largest organ and needs far more protection than we typically offer. Prevention of UV damage is the best assurance to prevent skin cancer and hyperpigmentation. Consulting an expert on treatment options to lighten dark spots is advised given the complexity of all types of hyperpigmentation. It is recommended to utilize the knowledge and assistance of an experienced medical provider to help you create a treatment plan to best suit your needs and achieve the best results.
References
Espósito, A. C., Cassiano, D. P., da Silva, C. N., Lima, P. B., Dias, J. A., Hassun, K., Bagatin, E., Miot, L. D., & Miot, H. A. (2022). Update on Melasma—part I: Pathogenesis. Dermatology and Therapy. https://doi.org/10.1007/s13555-022-00779-x
Gonzalez-Molina, V., Marti-Pineda, A., & Gonzalez, N. (2022). Topical Treatments for Melasma and Their Mechanism of Action. The Journal of Clinical and Aesthetic Dermatology, 15(5), 19–28. https://doi.org/https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9122278/
Goon, P., Banfield, C., Bello, O., & Levell, N. J. (2021). Skin cancers in skin types IV–VI: Does the Fitzpatrick scale give a false sense of security? Skin Health and Disease, 1(3). https://doi.org/10.1002/ski2.40
Ko, D., Wang, R. F., Ozog, D., Lim, H. W., & Mohammad, T. F. (2022). Disorders of hyperpigmentation. part II. Review of Management and treatment options for hyperpigmentation. Journal of the American Academy of Dermatology. https://doi.org/10.1016/j.jaad.2021.12.065
Maghfour, J., Olayinka, J., Hamzavi, I. H., & Mohammad, T. F. (2022). A focused review on the pathophysiology of post‐inflammatory hyperpigmentation. Pigment Cell & Melanoma Research, 35(3), 320–327. https://doi.org/10.1111/pcmr.13038
Praetorius C, Sturm RA, Steingrimsson E. Sun-induced freckling: ephelides and solar lentigines. Pigment Cell Melanoma Res. 2014;27(3):339-50. doi: 10.1111/pcmr.12232. [PubMed: 24517859].
Wang, Y., Zhao, J., Jiang, L., & Mu, Y. (2021). The application of skin care product in Melasma treatment. Clinical, Cosmetic and Investigational Dermatology, Volume 14, 1165–1171. https://doi.org/10.2147/ccid.s323748